
22 Mar Genetic testing and some treatments for hereditary breast and ovarian cancer syndrome (HBOC) are now covered by health insurance.
What is hereditary breast and ovarian cancer syndrome (HBOC)?
It is estimated that five to ten percent of breast and ovarian cancers are closely associated with hereditary factors.
In recent years, hereditary breast and ovarian cancer syndrome (HBOC) has been recieving more attention.
Characteristics of HBOC

- If you are a woman and have certain gene mutations (BRCA 1 or BRCA 2), you are at higher risk of developing breast, ovarian, and other cancers such as fallopian tube cancer and peritoneal cancer.
- If you are a man and have these mutations,you are at higher risk of developing breast, prostate, and pancreatic cancer.
What is DNA?
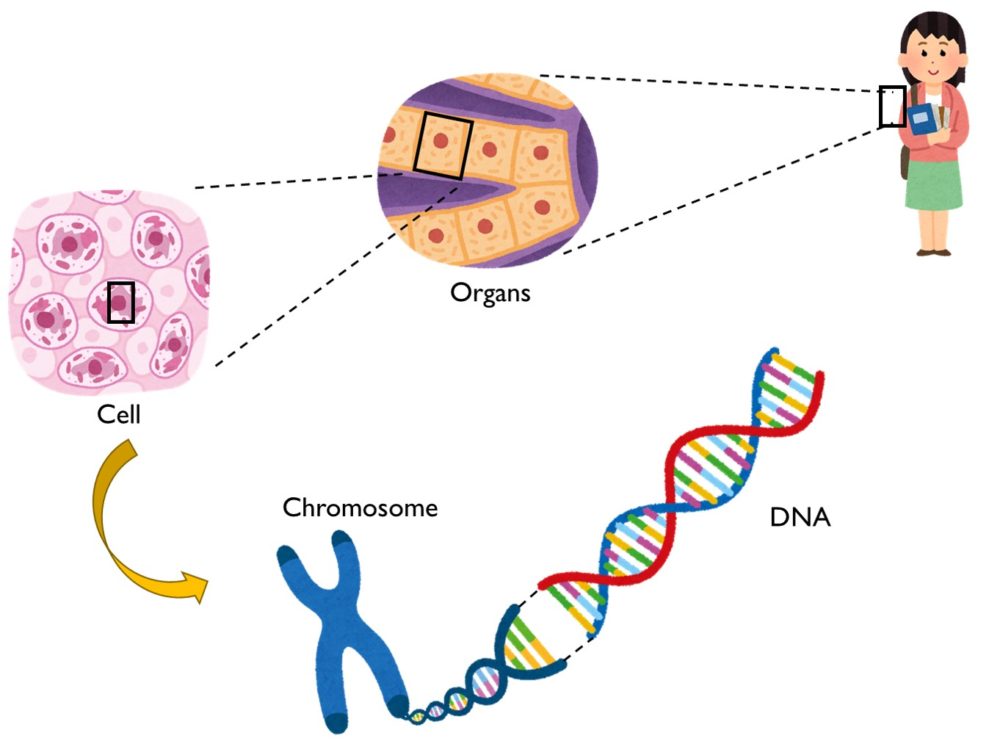
The nucleus of each human cell contains DNA. DNA acts as written instructions for creating genetic structures.
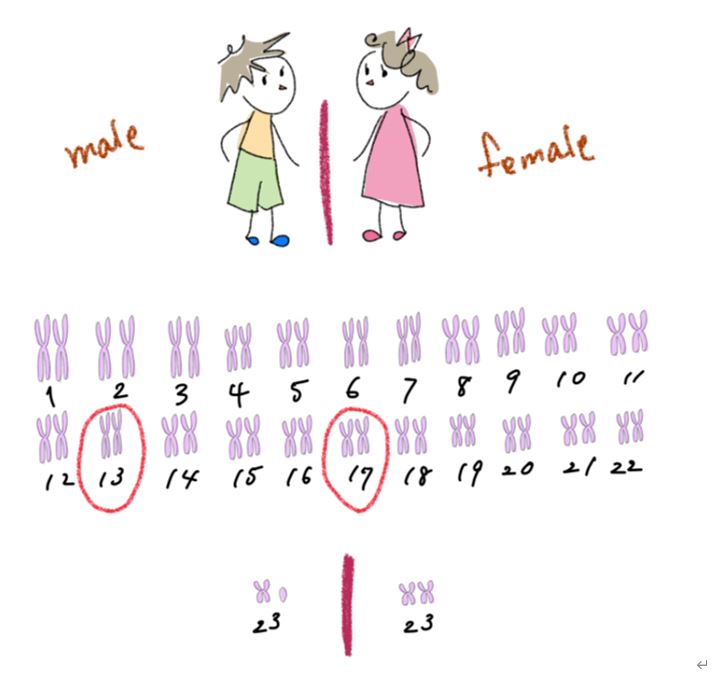
BRCA1 and BRCA2 genes are located on chromosome 13 and chromosome 17, respectively. If you are a carrier of one of these mutations associated with cancer risk, then HBOC is diagnosed.
What does it mean to have a BRCA mutation?
・It is known that inherited mutations in the genes, BRCA1 and BRCA2 are related to breast and ovarian cancer.
・However, not everyone who inherits a BRCA1 or BRCA2 mutation will get breast or ovarian cancer.
・In other words, some people may never develop either cancer in their lifetime, some may develop both cancers, and some may only develop one of the cancers. In addition to the genetic factors, environmental factors such as smoking also play a role in cancer development because they increase the cancer risk.
・The risk for developing cancer is reported below. Refer to the Japanese JOHBOC pamphlet.
|
BRCA1 Mutation |
46% to 81% lifetime risk for breast cancer 39% to 63% lifetime risk for ovarian cancer 8.6% risk by age of 65 years for prostate cancer 1 to 3% lifetime risk for pancreatic cancer
|
|
BRCA2 Mutation |
38% to 84% lifetime risk for breast cancer Up-to 8.9% lifetime risk for breast cancer (in males) 16.5% to 27% lifetime risk for ovarian cancer 15% risk by age of 65 years and 20% lifetime risk for prostate cancer 2 to 7% lifetime risk for pancreatic cancer
|
・Some, but not all, gene mutations are inherited by the next generation of a family.
・There is a 50% chance of parents passing these mutations on to their children due to autosomal dominant inheritance pattern.
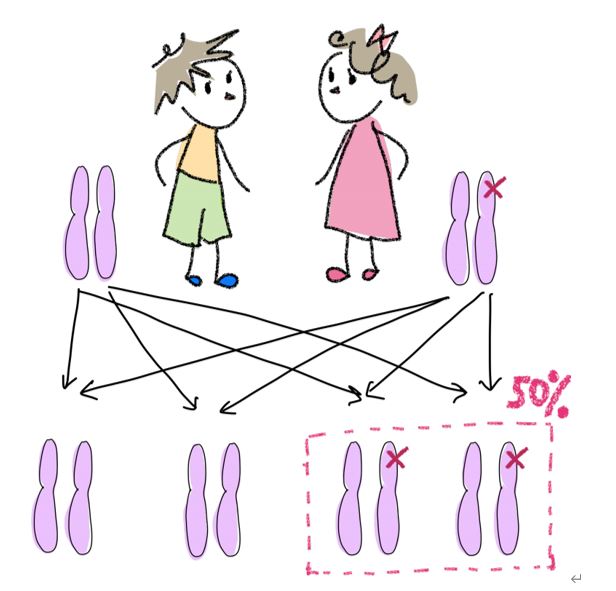
If a parent has a BRCA mutation known to cause hereditary breast and ovarian cancer,his/her children each have a 1 in 2 (50%) chance of having the same mutation.
What is genetic testing?
- Genetic testing is a test for your genes that identifies changes (mutations) may cause hereditary cancers. If a mutation is found, genetic testing can determine whether or not the mutation is associated with the development of cancer.
- The condition of your genes won’t change throughout your lives even if you make changes in your lifestyle, because hereditary genetic information is permanent. However, other environmental factors may increase your risk of developing cancer regardless of whether you have the genetic mutation.
Medical Cost
- Genetic testing for BRCA1 and BRCA2 may be covered by health insurance in some cases. If the testing is covered 70% by insurance, the cost to you will be about ¥60,000. If your case is not covered by health insurance, the cost varies depending on each medical facility. Please ask the medical staff for the specific cost.
In cases where BRCA1 and BRCA2 genetic testing is covered by health insurance.
If you have already developed breast or ovarian cancer and HBOC is suspected, you are eligible for the genetic testing covered by your health insurance.
— if you have:
- A personal history of breast cancer diagnosed at age 45 or younger.
- A personal history of triple negative breast cancer diagnosed at age 60 or younger.
- Two or more times primary breast cancer on the same breast diagnosed.
- A personal history of male breast cancer
- A personal history of ovarian cancer, fallopian tube cancer, or peritoneal cancer
- Possible carrier of BRCA1 or BRCA2 mutation showed by genetic testing using multigene panels
- A personal history of breast cancer and one or more relatives with breast cancer or ovarian cancer
- A personal history of breast cancer, ovarian cancer, or peritoneal cancer, and one or more relatives are known to be carrier of BRCA1 or BRCA2 mutation.
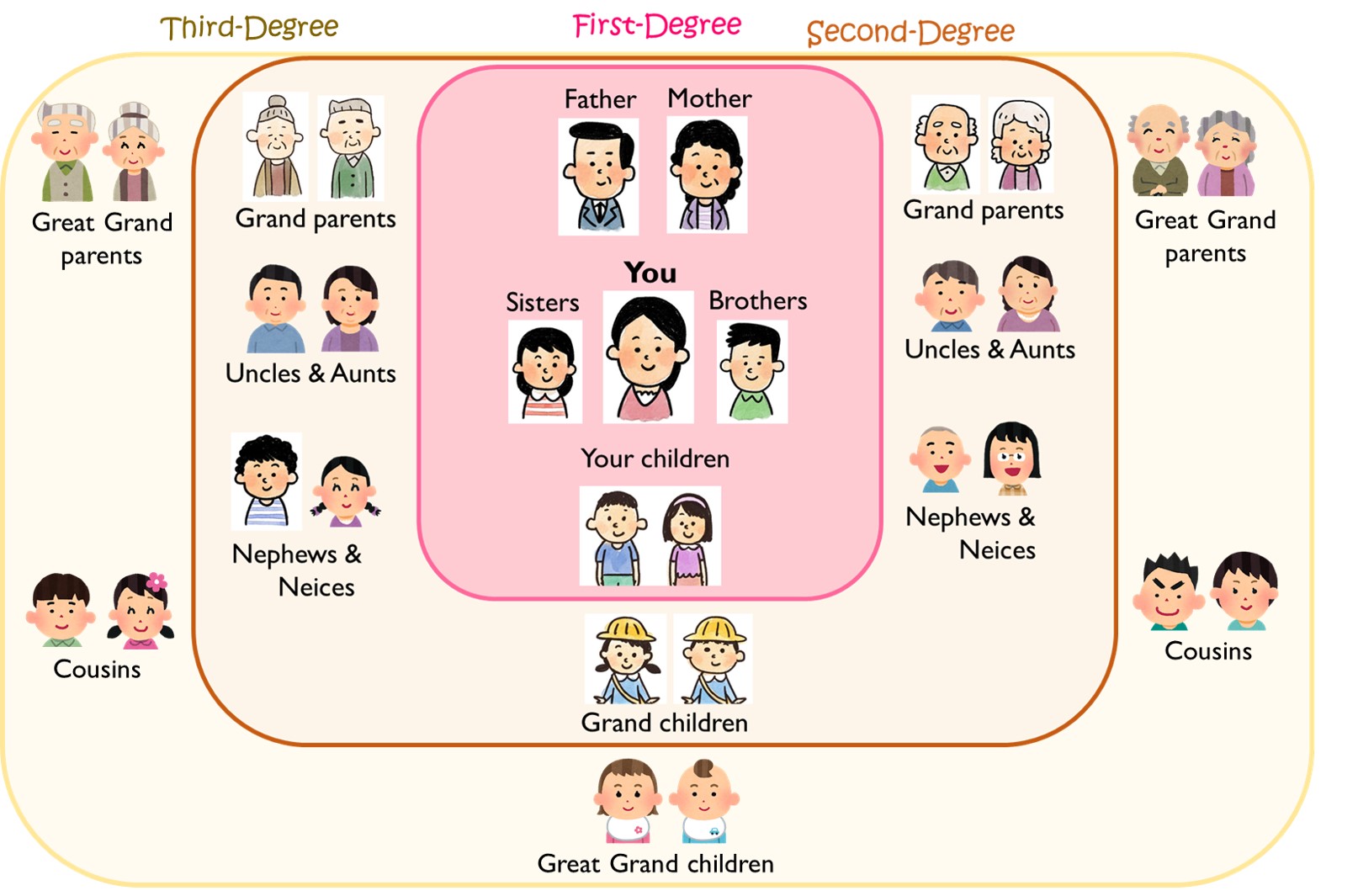 *Relatives include parents, siblings, siblings of stepparents, children, niece and nephew, paternal uncles and aunts, maternal uncles and aunts, grandparents, granduncles and grandaunts, cousins, grandchildren, etc.
*Relatives include parents, siblings, siblings of stepparents, children, niece and nephew, paternal uncles and aunts, maternal uncles and aunts, grandparents, granduncles and grandaunts, cousins, grandchildren, etc.
Genetic counseling
Genetic counseling before genetic testing for hereditary breast and ovarian cancer is important. If you have a personal medical history of breast cancer or ovarian cancer, first talk to your breast surgeon or your gynecologist. Ask him/her to refer you to medical facility with a genetic counselor, if HBOC is suspected.
Hospitals in Hokkaido, Designated by JOHBOC, for HBOC as of June 13, 2023
| Area | name of Facility | Website |
| Sapporo | Hokkaido University Hospital | https://www.huhp.hokudai.ac.jp/center_section/rinshoidenshi/ |
| Sapporo Medical University Hospital | https://web.sapmed.ac.jp/hospital/section/genetics/ev9eit0000005jnh.html | |
| Hokkaido Cancer Center | https://hokkaido-cc.hosp.go.jp/outpatient/index05.html | |
| Asahikawa | Asahikawa Medical University Hospital | https://idenshi.jp/ |
If you have a positive test result, several medical options are available.
The most effective option for preventing cancer is surgery to remove the breasts (mastectomy) and ovaries and fallopian tubes (salpingo-oophorectomy).
Reports from overseas indicate that 30-70% of BRCA mutation carriers have undergone Risk reducing salpingo-oophorectomy (RRSO).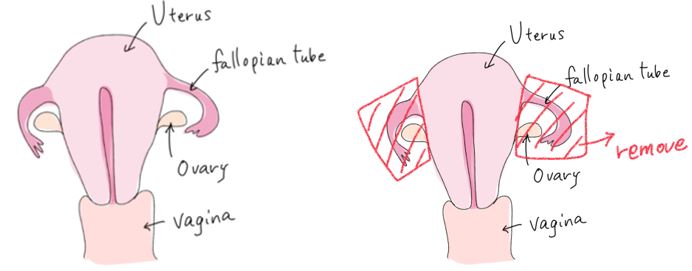
Risk reducing salpingo-oophorectomy (RRSO)
Surgery to remove both sides of the fallopian tubes and ovaries while there are no signs of cancer under diagnostic imaging. Incidence of ovarian cancer increases from about age of 40, it is recommended that RRSO should be performed by age of 50 if you have the positive genetic test result for BRCA1 or 2 mutations.
Risk reducing mastectomy(RRM)
Surgery to remove the breasts while there are no signs of cancer under diagnostic imaging. RRM reduces the risk of breast cancer by more than 90%. Because the incidence of breast cancer increases from about age of 30, it is recommended that RRM be performed by age of 40 if you have the positive genetic test result for BRCA1 or 2 mutations.
Masako Sohara M.D. (an Ob-Gyn doctor)
Refer to 遺伝性乳がん卵巣がん症候群(HBOC)をご理解いただくために ver.2020_1 by JOHBOC (in Japanese).


