02 Feb Chapter 4: What we want those just starting to have sexual intercourse to know セックスデビュー世代に知っておいて欲しいこと
The original content is here ⇒日本語
The right contraception?
Extra-vaginal ejaculation is not contraception.
It’s not “Ejaculate outside the vagina, and that should be fine!”
Have you ever had this experience? “We suddenly decided to have sex and we don’t have a condom! But if my partner withdraws his penis from the vagina before ejaculation, I won’t get pregnant, right?” Actually, it is possible to get pregnant with the withdrawal method (also called coitus interruptus).
Although the Cowper’s gland fluid (the so-called “precum”) itself, which is secreted through the urethra before ejaculation, does not contain sperm, a small amount of semen may pass out through the urethra. In addition, semen adhering to the vaginal perineum may enter the vaginal canal and travel up to the uterus.
Condoms are important as a means of preventing sexually transmitted diseases as well. Remember, protecting both of you is important.
Did you know that using condoms is not 100% effective as a method of contraception?
Condoms are a common method of birth control, but it is estimated that 2-18 women out of every 100 get pregnant each year, including those caused by incorrect and unsuccessful use of condoms. It is important to master the use of condoms because they are highly effective contraceptives when used correctly.
Let’s check “Common Incorrect Condom Usage”!
×Keep them in your purse.
Condoms are very delicate! Putting them in the same place as sharp or hard objects can damage them or cause them to deteriorate. Also, hot and humid environments can cause deterioration. When carrying them around, keep them in the original box or a hard case.
Condoms have an expiration date. Read the package and check it!
×The size is not right. 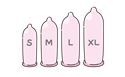
Just like clothing, condoms come in different sizes. If the size is not right, there is a risk of it tearing or coming off. Choose a condom that fits you by putting it on before having sex.
×Wrong side up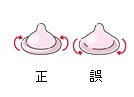
Condoms have two sides, inner and outer. If used incorrectly, they may tear due to friction. Both of you be sure to check together before putting the condom on. Also, do not reuse a condom just to avoid wasting it. Semen on a used condom can cause pregnancy.
◉Here’s the right way of using a condom!
Learn about the proper use of a condom from these illustrations! It is often thought that only men need to know how to wear a condom, but both of you are responsible for contraception.
Let’s learn together.
![]() 1.Push the contents of the package together before opening to prevent damage.
1.Push the contents of the package together before opening to prevent damage.
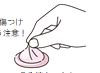 2.Pinch the tip of the condom and gently release the air.
2.Pinch the tip of the condom and gently release the air.
Don’t damage it with your fingernails!
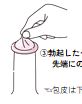 3.Place it on the tip of the erect penis.
3.Place it on the tip of the erect penis.
☜The foreskin should be pulled down.
|
If you have a tight foreskin (phimosis) which can be pulled back, make sure to wear a condom with the glans uncovered. |
Refer to Tight foreskin (phimosis) by NHS
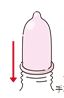 4.Roll it down once.
4.Roll it down once.
☜The foreskin is kept tucked underneath.
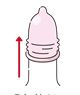 5.Roll it up with the foreskin.
5.Roll it up with the foreskin.
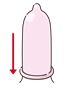 6.Roll it down once again, and that’s it!
6.Roll it down once again, and that’s it!
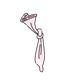 7.After ejaculation, tie the condom and discard it to prevent semen leakage.
7.After ejaculation, tie the condom and discard it to prevent semen leakage.
The contraception failed! What should I do・・・
You should visit a hospital or clinic to get a prescription for a morning-after pill to take within 72 hours.
Even if you are careful, contraception can fail due to condoms coming off or damage to the condom. Emergency oral contraceptives used after sexual intercourse to avoid pregnancy are called the morning-after pill. The most important thing is to take them within 72 hours of sexual intercourse that could result in pregnancy.
◆Where can I get them?
You can get a prescription at an OB-GYN clinic. If you need them after office hours, call the clinic first.
◆What is the process for prescribing the morning-after pill?
The doctor will ask you about your last menstrual period, if you had any sexual intercourse that could result in pregnancy, and, if so, the date and time (especially time). If it is within 72 hours, the doctor will prescribe the morning-after pill. Then, you will receive an explanation about taking it.
◆What about side effects?
You may experience nausea or headaches.
◆How much will it cost?
Prescriptions for contraception are not covered by insurance and cost around 5,000 to 20,000 yen, depending on the clinic.
◆When will we know if it’s working?
Successful contraception can be confirmed by menstrual bleeding within 3 weeks after taking the pill. However, since there is a possibility of irregular bleeding, a pregnancy test should be done both 2 weeks and 3 weeks after the last sexual intercourse. If both tests are negative, that rules out pregnancy almost 100%.
◆Can you avoid pregnancy 100%?
 The success rate of the morning-after pill decreases over time. It decreases even more when it is used around the day of ovulation. The morning-after pill is not a reliable method of birth control and is not for routine use.
The success rate of the morning-after pill decreases over time. It decreases even more when it is used around the day of ovulation. The morning-after pill is not a reliable method of birth control and is not for routine use.
The pill is a method of birth control which can be used by women on their own and which is more effective than condoms.
The morning-after pill is only for emergency use in the event of contraceptive failure or unprotected sexual intercourse. In contrast, the pill or oral contraceptive (OC) is a reliable method of contraception that can be used on a daily basis. According to the “Guidelines of the Japan Society of Obstetrics and Gynecology,” if a woman does not forget to take the pill, the probability of pregnancy is almost zero, making it a highly reliable contraceptive method that can be used by women on their own.
An OC is a contraceptive, but there is also an LEP (low dose estrogen progestin) that has the same active ingredients as an OC and is covered by insurance as a treatment for dysmenorrhea. (For more information, see Chapter 2 – “The Period Savior! Low-dose Pill“.) The patient pays completely for the OC. The monthly fee is about 2,000~3,000 yen and varies depending on the medical institution, so consult your OB-GYN first about a prescription.
For those who are “worried about forgetting to take the pill,” we recommend the intrauterine contraceptive (IUS). (→ Scroll down and see the column for details)
One Student’s Experience
“I don’t always remember to take the pill”. This is the reason why I chose Mirena (IUS). I talked to my doctor about my concerns about forgetting to take the pill, and we somehow ended up talking about Mirena…. The doctor told me that Mirena might be painful and difficult to insert if you’ve never had a baby before but then asked me “Do you want to give it a try?” and we managed to insert the device. I believe that I was able to choose a method for reducing menstrual pain and a type of birth control that suits me.
chose Mirena (IUS). I talked to my doctor about my concerns about forgetting to take the pill, and we somehow ended up talking about Mirena…. The doctor told me that Mirena might be painful and difficult to insert if you’ve never had a baby before but then asked me “Do you want to give it a try?” and we managed to insert the device. I believe that I was able to choose a method for reducing menstrual pain and a type of birth control that suits me.
Ask your OB-GYN doctor
Is it safe to have sex without contraception after taking the morning-after pill?
 It is not “once you take it, you are completely safe”.
It is not “once you take it, you are completely safe”.
If you have sexual intercourse again, there is a possibility of pregnancy.
The morning-after pill prevents you from being pregnant by delaying ovulation. Even after taking it, the chance of conception increases again.
You should abstain from sexual intercourse until your next period or use condoms properly.
Some women use the morning-after pill repeatedly, but please take this as a good opportunity to consider taking the pill, which is a more reliable birth control.
The success rate of the morning-after pill(contraceptive rate)may seem high, but that is only for a single act of sexual intercourse. On the other hand, using the pill results in almost no cases of pregnancy.
Column
Another Method of Birth Control Intrauterine System (IUS)
An intrauterine device (IUS) is also known as Mirena.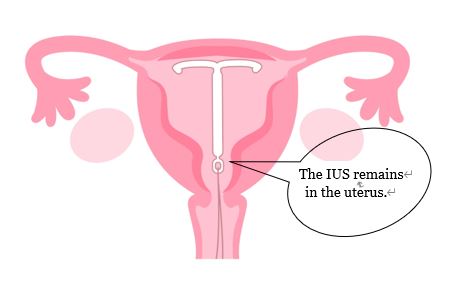
Its contraceptive efficacy is equal to or better than that of the pill. It has also been shown to be effective in reducing excessive menstrual periods/hypermenorrhea and pain, and when it is used as a treatment for dysmenorrhea and hypermenorrhea, the cost is covered by insurance.
◆Advantages
Long-term (about 5 years) contraceptive effects can be expected. Once you have the IUS inserted, you do not need to worry about forgetting to take it, like you might with the pill.
◆Disadvantages
For some women, it may come out spontaneously. Since it is implanted in the uterus, inserting one into women with a narrow cervix, such as those who haven’t given birth, might not be possible. There are individual differences, so please consult your obstetrician/gynecologist first.
◆Side Effects
Irregular bleeding may continue for several months.
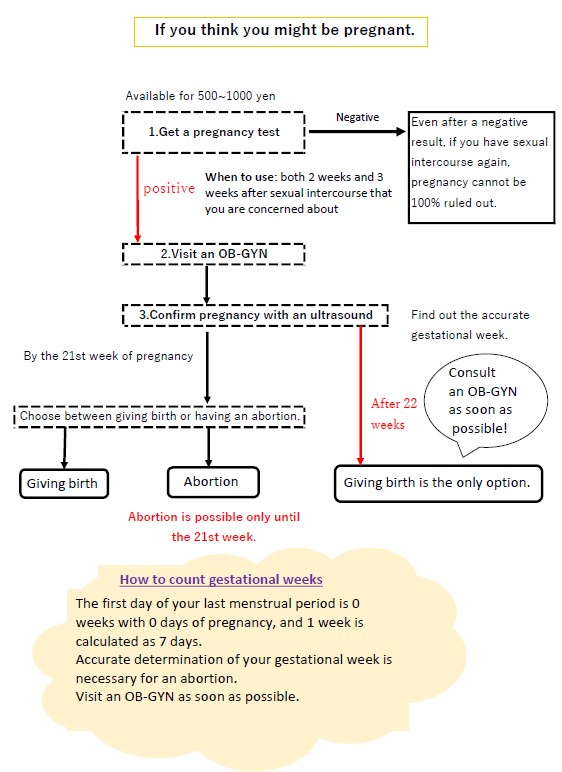
If you think you might be pregnant.
“I’m not getting my period.”
“I have symptoms like morning sickness.”
No matter how careful you are, you can still have an unexpected pregnancy. You may be filled with various anxieties and worries, such as, “Should I have the baby or not?” or “How much would an abortion cost?” If you or someone you love has an unwanted pregnancy in the future, please refer to this flowchart.
Q&A Ask your OB-GYN.
 Do I need my partner’s consent for an abortion?
Do I need my partner’s consent for an abortion?
Your choice is the one that is the most respected.
Basically, it is better to have your partner’s consent, but it is not mandatory. However, each OB-GYN doctor responds differently. Even if the partner does not consent, the woman’s choice is respected.
If you are a minor (under 18 years old), most medical institutions will ask for parental consent.
 Is surgical abortion safe?
Is surgical abortion safe?
Is it true that abortion makes it harder to get pregnant?
Yes, it’s safe in most cases, though it is still not 100% safe.
It does not make it difficult to conceive.
Although the operation is performed with the utmost consideration for the health of the mother, the risk is not zero. Possible complications during the surgery will be explained in advance. It will not make it difficult to conceive. However, repeated abortions can be a burden, not only physically but also mentally. Use reliable contraceptive methods on a regular basis.
conceive. However, repeated abortions can be a burden, not only physically but also mentally. Use reliable contraceptive methods on a regular basis.
 How much does a surgical abortion cost?
How much does a surgical abortion cost?
Do I need to be hospitalized?
For a surgical abortion on women less than 12 weeks pregnant, a dilation and curettage (D&C) or a vacuum aspiration is performed to remove the content of the uterus. For a pregnancy from 12 to less than 22 weeks long, a uterine contraction agent is used to induce labor and cause a miscarriage (stillbirth).
The cost is approximately 80,000-100,000 yen for a pregnancy less than 12 weeks long, and the cost for a pregnancy 12-21 weeks long is equivalent to that of giving birth, but it varies depending on the medical facility.
In general, hospitalization is required for a procedure performed after a  12-week pregnancy, but whether or not you need to be hospitalized depends on the medical facility.
12-week pregnancy, but whether or not you need to be hospitalized depends on the medical facility.


